hūmNET Pilot Outcomes Brief
Mar 12, 2026

Early Results from Healthcare & Recovery Community Validation Studies
Executive Summary
What We Measured: 88 participants¹ across two at-risk populations shared a few minutes of synchronous peer support focused on a phrase that let them know they were not alone, and reported their wellbeing before and after on a 0-100 struggling-thriving scale.
What We Found: Consistent 34-36 point improvement in wellbeing across both populations (healthcare workers and recovery community). 92-94% positive response. Strong peer-led growth indicators with participants expressing willingness to organize sessions for their colleagues.
What It Means: The results demonstrate a consistent, early efficacy signal across populations. While direct comparisons to other peer support interventions require controlled studies, these preliminary findings justify progression to institutional pilots that will measure engagement, retention, and operational impact.
Methodology
What is a humn? (Pilot Version)
A humn is a brief, synchronous peer support experience. In these validation studies, participants joined for 3-5 minutes of synchronized presence that included: a focus phrase chosen for their community, soothing vibration, immersive sound, a glowing ball that circles the focus words for gentle attention anchoring, and a real-time count of how many others were present in that moment.
Our validation studies were designed around this framework:
Population: Healthcare workers and individuals in recovery facing acute emotional distress -- patient deaths, moral injury, cravings, withdrawal stress.
Intervention: hūmNET delivers a 3-5 minute synchronous peer support experience combining focus phrases, haptic vibration, immersive sound, and real-time presence awareness.
Comparison: Solo wellness interventions (meditation apps, breathing work) address individual regulation. hūmNET adds the neurobiology of social synchrony and the "helper's high" -- mechanisms that create sustainable peer networks rather than extractive engagement.
Outcomes: Immediate wellbeing improvement, adoption intent, and peer-organizing willingness. Institutional pilots will measure sustained engagement, retention impact, and long-term clinical outcomes.
¹ Healthcare workers (N=51, July 2025) and recovery community members (N=37, August 2025), recruited via Prolific research platform.
Our hypothesis:
Our hypothesis rests on activating these mechanisms through brief moments of shared presence. Rooted in the neuroscience of social synchrony, these shared moments create measurable emotional alignment. Those in need feel held. Supporters get a microdose of altruism. Everyone leaves knowing--you're not alone.
Research demonstrates that "shared physiological states during social interactions create a biological foundation for empathy and mutual support" (Feldman, 2017). hūmNET creates these shared states through brief moments of shared presence.
Note: The full hūmNET platform will include additional features like a presence visualizer (glowing beacons on a live map), but these pilot results reflect the core intervention components only.
Evidence-Based Components
hūmNET’s design integrates multiple therapeutic modalities with established research foundations:
Haptic/Vibration Therapy: Research demonstrates that therapeutic vibration reduces anxiety and supports nervous system regulation. Participants report the vibration "feels soothing and really holds you." ¹ ²
Therapeutic Sound Design: Developed with guidance from experts in therapeutic sound applications, the platform uses immersive sound chosen to support emotional regulation, with planned integration of binaural beats and therapeutic frequencies. Meta-analyses indicate efficacy in reducing anxiety and fear.³
Mindful Focus Practices: Brief mindfulness interventions targeting sustained attention have strong neurobiological evidence. The platform's visual tracking provides gentle attention anchoring without cognitive burden. ⁴
Neuroscience of Social Synchrony: Shared presence and synchronized experiences create measurable emotional alignment through established neurobiological pathways. ⁵
Regenerative Altruism: Research on the "helper's high" shows that altruistic action measurably improves the helper's wellbeing, creating a regenerative support network. ⁶ ⁷

Note: While these individual components have strong research foundations, hūmNET's specific combination requires further study through our institutional partnerships.
Study Design
Both the Healthcare Worker and the Recovery Community studies followed the same approach:
Participants recruited through Prolific research platform (Prolific is the highest-ranked platform for academic research quality).
Asked to recall a challenging moment and rate their wellbeing on a self-reported scale (0=struggling, 100=thriving).
Joined a humn experience using the phrase "You're not alone. We can get through this." (3-5 minutes).
Asked to note how many others were present during the experience.
Self-rated their wellbeing immediately after and shared a reflection.
Populations Studied
Healthcare Workers (N=51): Study conducted July 2025. All 51 participants confirmed consistent group experience and were included in analysis. Participants represented a diverse cross-section of clinical roles:
59% Nurses (RNs, LPNs, Charge Nurses)
18% Doctors (MDs, DOs)
14% Mental Health Professionals (Psychologists, Social Workers)
9% Other Healthcare Fields (EMS, etc.)
Real challenges reported: patient deaths, burnout, workplace trauma, compassion fatigue.
Prior phrase testing surfaced "You're not alone. We can get through this." as most helpful (80%).
Recovery Community (N=37): Study conducted August 2025. 49 participants recruited across recovery stages; 37 confirmed with consistent group experience (2+ others present during session) and included in primary analysis. Participants spanned the recovery journey:
49% early recovery
22% currently using substances
22% sustained recovery
5% MAT participants
Substance types: alcohol, opioids, stimulants, cannabis (often poly-substance). Real challenges: cravings, withdrawal, relationship stress, family trauma.
Phrase testing note: while "One day at a time" was most resonant for this community, the pilot used "You're not alone. We can get through this." for consistency across populations.
What We Measured
Primary outcome: Change in self-reported wellbeing on 0-100 struggling-thriving scale. Secondary outcomes: Adoption intent, willingness to organize sessions for peers, qualitative feedback.
Study Context & Limitations
Participants were recruited via the Prolific research platform and self-reported current challenges. Outcomes were measured immediately pre- and post-intervention using a subjective wellbeing scale. Results reflect short-term impact. This study did not assess durability, clinical outcomes, or long-term behavior change.
What We Found
Healthcare Worker Results

+36 Point Average Improvement
Pre-humn: 21.5 average
Post-humn: 58.0 average
This represents a +36 point average improvement (169% increase) on a 0-100 wellbeing scale following a single 3-5 minute session.
94% Positive Response
48 participants (94%) felt measurably better. Only 2 participants (4%) experienced decreased wellbeing.* 1 participant (2%) reported no change.
_____________________________________
*Critical Product Insight: One participant who did not improve identified as autistic and reported the sound felt like voices and was disturbing "like in a horror movie." This feedback was invaluable, directly validating the roadmap requirement for granular sensory customization in the enterprise version. The participant "loved" the concept but could not tolerate the current sound design.
69% Would Use If Employer-Provided
Strong workplace demand signal: 26% "very likely" + 43% "likely" to use regularly if their hospital or health system offered it.
Strong Peer-Led Growth Indicators
23 participants (45%) signed up to organize a humn for their peers. Participants who volunteered to organize estimated inviting an average of ~10 colleagues, indicating strong peer-driven growth potential (4.3x viral coefficient) if implemented institutionally.
What They Said
"More relaxed and weirdly peaceful." -- RN (Community Nursing), Male, 38, +60 point improvement
"That vibration and sound is very soothing, it helps ground you." -- Nurse, Female, 34, +25 point improvement
"I feel a slight peace of calm and joy" -- Mental Health Practitioner (describing burnout with facial numbness before the humn), Social Worker, Female, 41, +46 point improvement
"I feel pretty good, i was worried for my shift today but now i feel in control, regardless of what the day throws at me. I do feel the humn vibration and sound is a good reset for my nervous system." -- Nurse, Female, 40, +81 point improvement
Who They Were
Average age: 34 years (range 22-63). 71% female, 27% male. 26% have ongoing mental health conditions. 62% practice meditation regularly. Mixed ethnic representation. Strong response across all clinical specialties and experience levels.
Recovery Community Results

+34 Point Average Improvement
Pre-humn: 27.8 average
Post-humn: 61.4 average
This represents a +34 point average improvement (121% increase) on a 0-100 wellbeing scale following a single 3-5 minute session.
92% Positive Response
34 participants (92%) experienced positive improvement in wellbeing following the humn experience.
78% Would Use If Recovery Program Provided
Strong adoption intent across all recovery stages--from currently using through sustained recovery.
Strong Peer-Led Adoption Intent
67% of participants expressed interest in organizing a humn for others in recovery, estimating they would invite an average of ~10 peers each (9.7). This represents a viral coefficient of 6.5x, significantly higher than the 4.3x seen in healthcare, confirming the powerful "regenerative" nature of the recovery community.
What They Said
"I am feeling calm and relaxed, and pretty good thinking about how far I've come." -- Early Recovery (Alcohol), Female, 37, +18 point improvement
"I feel pretty good at ease and relaxed, confident" -- MAT Participant (Opioids/Stimulants), Female, 33, +41 point improvement
"It was an interesting experience. I think the sensory inputs helped distract me, focus my thoughts... It was interesting to think about 4 people there with me, hands and ears vibrating, going through their own journeys." -- Sustained Recovery (Alcohol/Cannabis/Tobacco), Male, 40, +15 point improvement
Who They Were
Diverse recovery stages:
41% Early Recovery (<12 months)
27% Currently Using Substances
16% MAT Participants (Medication-Assisted Treatment)
14% Sustained Recovery (12+ months)
2% Other/Transitional
Substance Type Representation:
Poly-substance use: Reported by 86.5% of participants.
High-risk populations: Well represented, with 60% reporting stimulant history, 49% alcohol, and 46% opioids.
Cross-Stage Reach: The positive response from currently using participants and those in MAT (43% combined) suggests the experience resonates across the full recovery spectrum, indicating it may offer meaningful support even for high-acuity populations.
Synthesis + What This Validates
The following table synthesizes the results across the two populations.
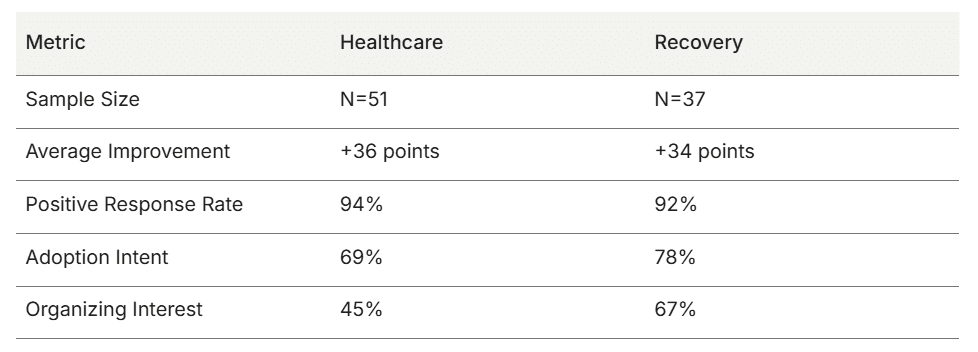
The numbers indicate a clear pattern: brief peer support creates measurable mood improvement regardless of the crisis context. The data supports the underlying mechanism.
Breadth of Applicability
Same intervention. Different populations. Different challenges. Consistent results.
Healthcare workers facing burnout, compassion fatigue, and professional grief responded just as strongly as people navigating substance use recovery--from active use through sustained recovery. This indicates that the core insight (synchronous peer support reduces isolation and improves wellbeing) may apply across contexts.
Community-Specific Content May Unlock Additional Impact
Remarkably, the recovery cohort achieved strong results (+34 points) using a universal phrase that only 47% rated as most helpful. With 67% preferring "One day at a time," community-specific content offers a clear opportunity to amplify these outcomes further.
Peer-Led Growth Signal Observed
45-67% of participants willing to organize sessions for their peers. This represents genuine altruistic motivation to extend support. The regenerative model--helping others helps you--shows early evidence of creating sustainable peer support networks.
Join us. Let's build the worldwide web of empathy!
Contact: Darren Mark, Founder & CEO Darren@humnet.live
Reviewed by: Enna Lamarre-Theodore DNP, RN, PMH-BC
Dr. Lamarre-Theodore is a global healthcare professional with more than 25 years of experience in Nursing, with a focus on wellness, mental health, and behavioral health. An advocate for caring and humanistic practices, embracing a transformational, collaborative, and multidisciplinary approach towards positive outcomes.
References
Fooks, C., & Niebuhr, O. (2024). Effects of Vibroacoustic Stimulation on Psychological, Physiological, and Cognitive Stress. Sensors, 24(18), 5924
Campbell, E. A., Hynynen, J., Burger, B., & Ala-Ruona, E. (2019). Exploring the use of Vibroacoustic treatment for managing chronic pain and comorbid mood disorders: A mixed methods study. Nordic Journal of Music Therapy, 28(4), 291–314
Garcia-Argibay, M., Santed, M. A., & Reales, J. M. (2019). Efficacy of binaural-beat perception on anxiety, fear, and pain: A meta-analysis. Psychological Research, 83(2), 357-372.
Zeidan, F., Johnson, S. K., Diamond, B. J., David, Z., & Goolkasian, P. (2010). Mindfulness meditation improves cognition: Evidence of brief mental training. Consciousness and Cognition, 19(2), 597-605.
Feldman, R. (2017). The neurobiology of human attachments. Trends in Cognitive Sciences, 21(2), 80-99.
Inagaki, T. K., & Eisenberger, N. I. (2016). The neurobiology of giving support. Psychosomatic Medicine, 78(4), 443-453.
Post, S. G. (2005). Altruism, happiness, and health: it's good to be good. International Journal of Behavioral Medicine, 12(2), 66-77.
© 2025 humNET. All rights reserved.